"We Brought Our Culture Here with Us": A Qualitative Study of Perceptions of HPV Vaccine and Vaccine Uptake among East African Immigrant Mothers
Fred Hutchinson Cancer Research Center (Ko, Taylor, Do); University of Washington School of Public Health (Ko, Taylor); University of Washington (Mohamed, Gebeyaw, Ibrahim, Winer); Somali Health Board (Mohamed, Ibrahim, Ali)
In the United States (US), adolescent human papillomavirus (HPV) vaccination coverage lags behind the Healthy People 2020 target of 80%. HPV vaccine uptake may present distinct challenges due to issues such as adolescent involvement in decision-making together with parents and providers, misconceptions about efficacy and safety, and cultural beliefs that vaccines normalise premarital sexual activity. This study explores how perceptions of, and decisions around, HPV vaccine uptake are shaped among Somali, Ethiopian, and Eritrean mothers of 11- to 17-year-old children in King County, Washington State, US.
Three focus groups - one each in Somali, Amharic, or Tigrinya (9-11 mothers per group, n=30) - were conducted from February 2017-April 2017 to inform development of a multi-level communication intervention to promote adolescent HPV vaccination. Intervention components included comic books for adolescents, educational forums for mothers, and an online continuing medical education (CME) course for providers. Focus groups were structured to unveil factors that shape individuals' perceptions and uptake of HPV vaccine and to provide feedback on comic book content and the interactive educational forums.
Two theoretical frameworks informed the development and analysis of a moderator guide, and the results of the investigation are organised accordingly:
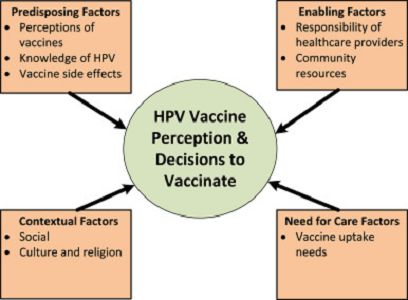
- Andersen's Behavioral Model of Health Services, which proposes that health services utilisation is determined by 3 factors:
- Predisposing factors - Across groups, many women indicated general concerns about vaccines and associated vaccination with disease risk. Risk perception was shaped by healthcare experiences in home countries. Most women did not know about the HPV vaccine. When the moderator explained that transmission was via sexual contact, some expressed concerns regarding children's sexual behaviour and abstinence. There was an overall sentiment of fear for vaccine side effects.
- Enabling factors - There was consensus that providers need to engage parents in communicating about the vaccine. Across all groups, women shared the need for information from multiple sources, including healthcare providers or media (e.g., DVDs. The Somali women emphasised the need to receive information by word of mouth.
- Need for care factors - Mothers discussed how their need for HPV vaccination is elevated when they are informed of the vaccine's purpose, importance, efficacy, and side effects. Women also stated that a strong recommendation from a co-ethnic or culturally sensitive provider elevated their need for vaccination.
- The Socio-Context Framework, which consists of the contextual forces that shape day-to-day experiences that directly and indirectly affect health behaviour, including:
- Social factors - The social influence women exert with one another in their daily lives through shared experiences emerged in all groups. Women also discussed how their friends serve as sounding platforms to validate or invalidate doctors' recommendations, with friends' advice trumping doctor recommendations.
- Cultural and religious factors - In all groups, women shared that it was culturally unacceptable to engage in discussions about sex with their children and that "anything that has to do with man and woman relationship is a secret". An Eritrean woman noted that their health behaviours in the US are shaped by their culture.
These findings suggest that providers should be aware of strong, pervasive vaccine mistrust among some members of the East African communities and that they should address vaccine safety when communicating about the HPV vaccine. Providers may want to connect with East African mothers at a level familiar to them (for example, shared goals to protect their child's health) and view mothers beyond the role of a patient's mother, but also a potential "social influencer" who can champion vaccine uptake in the community.
To increase awareness of the HPV vaccine, the researchers highlight the role of community-trusted sources, such as churches and community centres, as well as the use of electronic media and word of mouth to inform parents and peer-based education for their children. Rather than providing generic information on the HPV vaccine, inclusion of universal metaphors, such as the use of water to note a vaccine, may have stronger cultural resonance to East African women.
Papillomavirus Research 7 (2019): 21-25. https://doi.org/10.1016/j.pvr.2018.12.003
- Log in to post comments












































