"We're Potentially Worsening Health Inequalities": Evaluating How Delivery of the 2022 London Polio Booster Campaign Was Tailored to Orthodox Jewish Families to Reduce Transmission Vulnerability
London School of Hygiene & Tropical Medicine (Kasstan, Mounier-Jack, Chantler); National Health Service England (Zuriaga-Alvaro, Weil); United Kingdom Health Security Agency (Weil)
"Results indicate a need to conduct sustained public engagement activities and to work closely with community stakeholders to ascertain effective messaging strategies that can engage Haredi residents with accurate evidence of risk and levels of sensitivity, and via suitable dissemination pathways."
A 2022 polio booster campaign seeking to reach all children aged 1-9 across London, United Kingdom (UK) was part of a national enhanced poliovirus incident response following multiple detections of vaccine-derived poliovirus type 2 (VDPV2) isolates. Orthodox Jewish (OJ) children were particularly vulnerable to transmission due to disparities in childhood vaccination coverage and the transnational spread of poliovirus affecting linked populations in New York and Israel. This study aimed to evaluate how the polio booster campaign was tailored to increase uptake and enable access for OJ families in northeast and north central London boroughs. Specifically, it examined: how the polio booster campaign was communicated, implemented and delivered; how parents engaged with the campaign (and childhood immunisation services more broadly); and the impact of the campaign on documented disparities in routine childhood vaccination coverage in these areas.
The boroughs of Hackney and Haringey, which are the focus of the study, are home to a broad range of populations, and disparities in vaccine uptake are not specific to Haredi minorities. Yet, the 2014-16 World Health Organization (WHO) Tailoring Immunisation Programme (TIP) study conducted in north London documented widespread delayed acceptance among Haredi families in Hackney, as well as barriers to accessing vaccines. Haredi Jewish groups are distinguished by differences in customs that influence social organisation and how religious law (halachah) is interpreted.
This evaluation focuses on the period August 10 2022, when the campaign was announced, to December 23 2022, when the offer of a polio booster vaccine was withdrawn. Methods consisted of: (i) semi-structured in-depth interviews (n=36) with participants involved in the implementation and delivery of the polio booster campaign, as well as OJ mothers; (ii) site visits to 5 vaccination delivery points across Hackney and Haringey that were involved in the polio booster campaign; and (iii) rapid interviews (n = 26) to explore parental perceptions of the poliovirus incident and childhood immunisations.
The results are organised into three main themes:
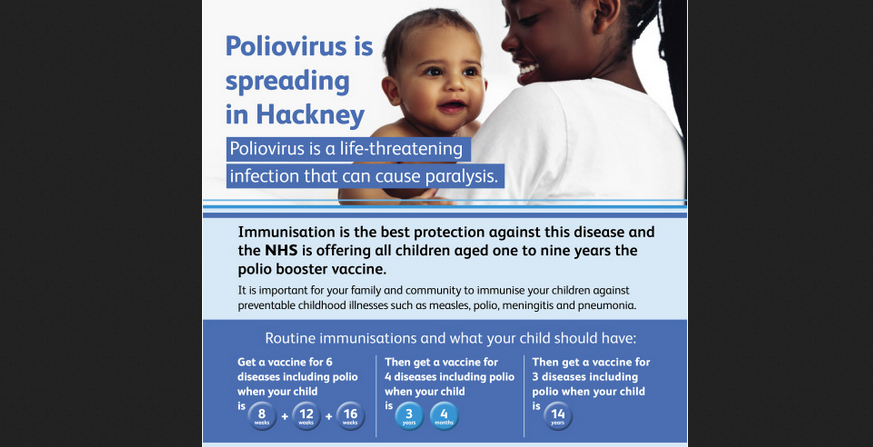
I) How the campaign was communicated: National communications produced by the United Kingdom Health Security Agency (UKHSA) conveyed that "Most of the UK population will be protected from vaccination in childhood, but in some communities with low vaccine coverage, individuals may remain at risk". This message was intended for the national audience, but required tailoring at regional (London) and borough levels by relevant stakeholders (e.g., local authority public health teams, which supported the tailored delivery of communications and engagement activities, signaling a coordinated response.). Healthcare provider (HCP) participants, however, felt the campaign messaging was not conducive to promoting urgency to vaccinate. The booster campaign was advertised via street posters across Hackney to convey localised transmission risk "(Poliovirus is spreading in Hackney"). National, regional, or local communications did not explicitly detail that Jewish families were vulnerable to the transnational spread of VDPV2 to avoid being stigmatising. Local-level material was produced to engage intended beneficiaries with the campaign. From mid-September 2022, a childhood immunisation coordinator based in Hackney developed targeted flyers to advertise key messages focused on polio transmission, and weekly vaccine clinics advertised in a pamphlet (supported by local authority public health). Parents attending for childhood vaccinations had engaged with these communications.
II) How the campaign was implemented and delivered via tailored means for Haredi families: Implementation in Hackney occurred via Primary Care Networks (PCN), which are consortia of general practitioner (GP) surgeries and community health services in specific localities, and 2 hospital hubs (ages 5-9). Convenience was crucial to engage Haredi families with the campaign, with primary care and community-delivery pathways the most practical vaccination sites and the offering of flexible clinic times critical. On the other hand, digital booking systems were a barrier. Parents interviewed as part of the evaluation were aware of the polio incident but did not consider their children to be at risk of transmission. Mothers who were unsure about the campaign turned to their social networks to deliberate, which tended to reinforce the perception that the booster was not necessary. Not all parents felt fully informed about the purpose of the polio booster campaign, and concerns surrounding past outbreak vaccination campaigns also influenced perceptions of the polio incident response. Hence, vaccine delay was not always due to access barriers.
III) The impact of the booster campaign in a context of lower-level routine childhood vaccination coverage: Some of the HCPs interviewed raised concerns of delays in targeted engagement with underserved populations during the campaign, which were linked to coordination of tasks across health partners. While Haredi families were considered a priority in the campaign response, public health (PH) participants were uncertain whether tailored activities initiated in Hackney were translating into measurable percentage increases in vaccine uptake. Local PH and HCP participants raised concerns that the resources required to deliver the campaign could have been directed to under and un-immunised child populations to more effectively address disparities in vaccination uptake between populations.
In discussing the findings, the researchers stress that, while often described as a "community", Haredi parents had diverse requirements as well as expectations of childhood vaccination services. However, on the whole, enablers to participating in the booster campaign for Haredi parents included targeted communications (in print, circulated to households via the Heimisher weekly pamphlet) and local-level delivery points on Sundays. Parents perceived a complementary delivery pathway, embedded in a community setting, as more family friendly when attending with multiple children.
Priorities emerging from this evaluation include: (i) developing messaging strategies with communities that effectively convey transmission risk and urgency to vaccinate while avoiding stigmatisation and (ii) strengthening primary care and valued delivery pathways to improve persistently low coverage rates.
UKHSA announced on March 23 2023 that the National Health Service (NHS) would deliver a second-phase catch-up campaign in London to reach "the most vulnerable children" aged 1-11, which includes children who are unvaccinated or have missed routine vaccinations, through a combination of primary care, primary schools, and community clinics. "Jewish minorities in London particularly in Hackney, maintain low vaccination coverage and close social networks in Israel, underscoring the need to effectively and efficiently engage parents with the second phase catch-up campaign."
SSM - Qualitative Research in Health, 100365.
- Log in to post comments












































