Correlation between Family Physician's Direct Advice and Pneumococcal Vaccination Intention and Behavior among the Elderly in Japan: A Cross-Sectional Study
Tsukuba Central Hospital (Higuchi); Kikugawa Municipal General Hospital (Narumoto); Shizuoka Family Medicine Residency Program (Narumoto, Inoue); Yu Pharmacy (Goto); Hamamatsu University School of Medicine (Inoue)
Because it lowers the risks of invasive pneumococcal disease and pneumococcal pneumonia, the 23-valent pneumococcal polysaccharide vaccine (PPSV23) is highly recommended for the elderly, but its uptake is low in Japan. This study aims to investigate the association between family physicians' recommendations for PPSV23 during outpatient care and PPSV23 vaccination intention and behaviour in the elderly.
The researchers explain that, among the principles in family medicine, using illness visits as opportunities for preventive medicine - and, by extension, to have conversations about this with patients - is important to achieve comprehensive care. As outlined here, due to medical service fees and limited time for discussion, the focus in outpatient encounters in primary care is typically more on providing laboratory tests and treatments. When examining geriatric patients, primary care physicians are frequently tasked with managing not only polypharmacy and multimorbidity but also newly developed acute health issues within the constricted outpatient time. It is possible that those factors, among others, make it challenging for family physicians to practice preventive medicine.
Beginning on November 1 2013, the researchers conducted a cross-sectional study with a questionnaire at a family medicine clinic in a rural community of Japan with a population of approximately 50,000 people. The participants were over the age of 65 without dementia who had maintained a continuity with the clinic. The questionnaire inquired PPSV23 vaccination status, the family physician's advice for PPSV23, socio-demographics, and the constructs in the Health Belief Model (HBM). The researchers defined those who had had vaccination intention and behaviour at the time of the investigation as "PPSV23 vaccinated group" and those who had no vaccination and uncertainty about being (or no intention to be) vaccinated in the future as "PPSV23 unvaccinated group". They used chi-square test for correlation between the physician's advice and PPSV23 vaccination/intention, univariate and multivariate logistic regression analysis for factors related to the vaccination/intention, and descriptive analysis for reasons for reluctance to the vaccination.
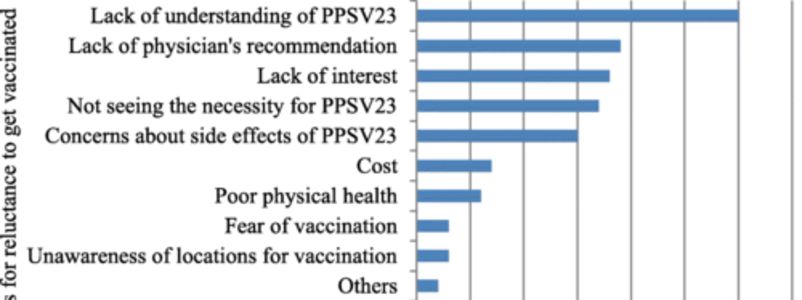
Of the 209 valid responses analysed, there were 142 participants in the PPSV23 vaccinated group and 67 in the PPSV23 unvaccinated group. The PPSV23 vaccination group was more likely to have had their physician's advice (80.2% vs 21.3%, p <0.001). Multivariate logistic regression analysis showed a significant association between PPSV23 vaccination and their physician's recommendation (odds ratio (OR) 8.50, 95% confidence interval (CI) 2.8-26.0), awareness of PPSV23 (OR 8.52, 95%CI 2.1-35.0), and the perceived effectiveness of PPSV23 (OR 4.10, 95%CI 1.2-13.9). The reasons for reluctance to get vaccinated included lack of understanding of PPSV23, lack of physician's recommendations, and concerns about side effects of PPSV23.
Considering the finding that a family physician's recommendation was positively correlated with PPSV23 vaccination intention and behaviour in the elderly, this study reinforces the importance of providing preventive services during time-constrained outpatient care, even in medical systems where it is undervalued. The study investigated the presence or absence of "family physician's direct recommendations", and did not explore doctor-patient communications, which could influence the patient's decisions to get vaccinated.
In conclusion: "In order to improve the PPSV23 vaccination rate at the individual level, it is essential to provide information on PPSV23 with better understanding of patient's perception of the vaccine, using any illness visit as an opportunity for preventive medicine."
BMC Family Practice (2018) 19:153. https://doi.org/10.1186/s12875-018-0841-3.
- Log in to post comments












































