Evaluation of Graphic Messages to Promote Human Papillomavirus Vaccination among Young Adults: A Statewide Cross-Sectional Survey
University of Minnesota
Communication studies have shown that not only do public service announcements or motivational messages evoke a variety of emotional responses, but that the emotional response can either inhibit or enhance persuasion. The objective of this study was to determine the most appealing human papillomavirus (HPV) vaccine promotion social media graphic for young adults 18-26 years of age in a large Minnesota, United States (US)-based convenience sample.
The United States Advisory Committee on Immunization Practices recommends administration of HPV vaccine for males and female ages 9 to 26 years, yet only 65% of females and 56% of males in the US initiate the vaccine series, and even fewer have completed the 2- to 3-shot series. Those at the older range of this scale are a particularly challenging group to reach, as they are beginning to make autonomous healthcare decisions and less frequently seek preventive health services compared to other age groups. Thus, the oft-endorsed strategy of increasing and improving the quality of healthcare providers' vaccine recommendations is unlikely to be sufficient to increase population coverage of HPV vaccination among this group. In contrast, they have a high prevalence of social media use, which could be leveraged to provide healthcare recommendations. Social media users spend very little time looking at each post, and graphics grab attention faster than text; therefore, this study sought to optimise social media graphics in order to increase the reach and potential impact of social media messaging around HPV vaccination for young adults.
A total of 1,037 participants 18-26 years of age completed a 36-item survey including information on demographics, HPV vaccination status, and eHealth literacy. One finding: Most participants reported using more than one social media app, but only 18% reported seeing information about HPV vaccine on social media. Among this subgroup, 23% felt that it was geared toward the young adult age group. While 43% found the information helpful, only 22% rated it as eye-catching, and 24% found it interesting. Only 19% found it easy to understand. Almost half (46%) recalled seeing social media messaging in support of the vaccine, and 5% recalled messaging against the vaccine.
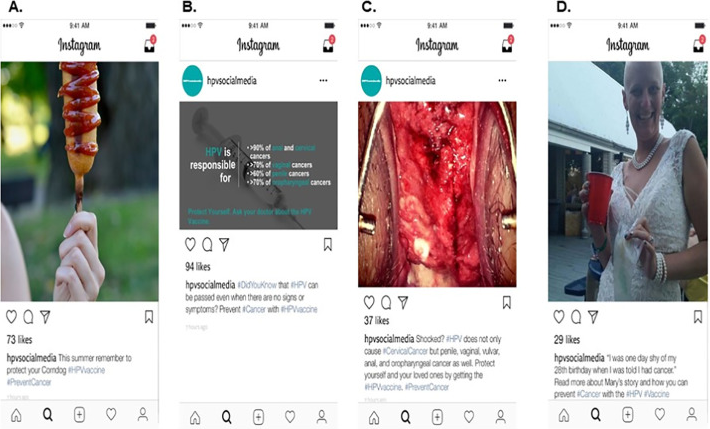
Participants also assessed the appeal of 8 Instagram graphic mock-ups promoting HPV vaccination to prevent cancer. (The researchers chose Instagram because, nationally, it is the most-used social media app among young adults age 18-29 years.) The graphics represented 4 categories: 1) infographics, since such graphics are often used by professional health organisations advocating for HPV vaccination; 2) disease photos attempting to elicit fear or disgust; 3) young adult cancer patient photos attempting to elicit sadness; and 4) humourous graphics attempting to elicit happiness. Each mock-up had Instagram-style text encouraging HPV vaccination to prevent cancer (e.g., "This summer remember to protect your corndog #HPVvaccine #PreventCancer", with a photo of a corndog). For each image, a survey question asked, "If this message showed up in your Instagram feed how likely is it that you would stop to read it?" Response options ranged from "very unlikely" (1) to "very likely" (5).
When asked how likely they would be to stop and read the study-generated Instagram messages, ratings for the individual images ranged from 2.6 ± 1.1 (patient photo) to 3.4 ± 1.1 (humourous graphic). Respondents rated the humourous graphics (pair mean rating 3.3 ± 1.0) and infographics (3.2 ± 1.1) statistically significantly higher than the disease graphics (2.9 ± 1.3) and patient photos (3.0 ± 1.0; p < 0.001 for pairwise comparisons). Nonetheless, the mean likelihood ratings on a 5-point Likert scale for the 4 graphic types were clustered around the "neutral" response option.
In short, the study showed statistically significant differences in response to the different graphic categories, but small effects suggest that the findings are unlikely to have significance for clinical or public health practice. The study does suggest avenues for additional research; for example, studies could evaluate whether the role of social media is limited to increasing knowledge of the topic or whether it has the potential to increase HPV vaccine uptake.
In conclusion: "factors other than optimal graphics, such as vaccine framing, may be more important in maximizing message appeal. Future social media health campaigns need to be tailored to appeal to adolescents and young adults from a variety of backgrounds, with a variety of graphics, messaging, topics, and utilization of a mixture of social media apps."
Preventive Medicine Reports, Volume 13, March 2019, Pages 256-261. https://doi.org/10.1016/j.pmedr.2019.01.002
- Log in to post comments












































